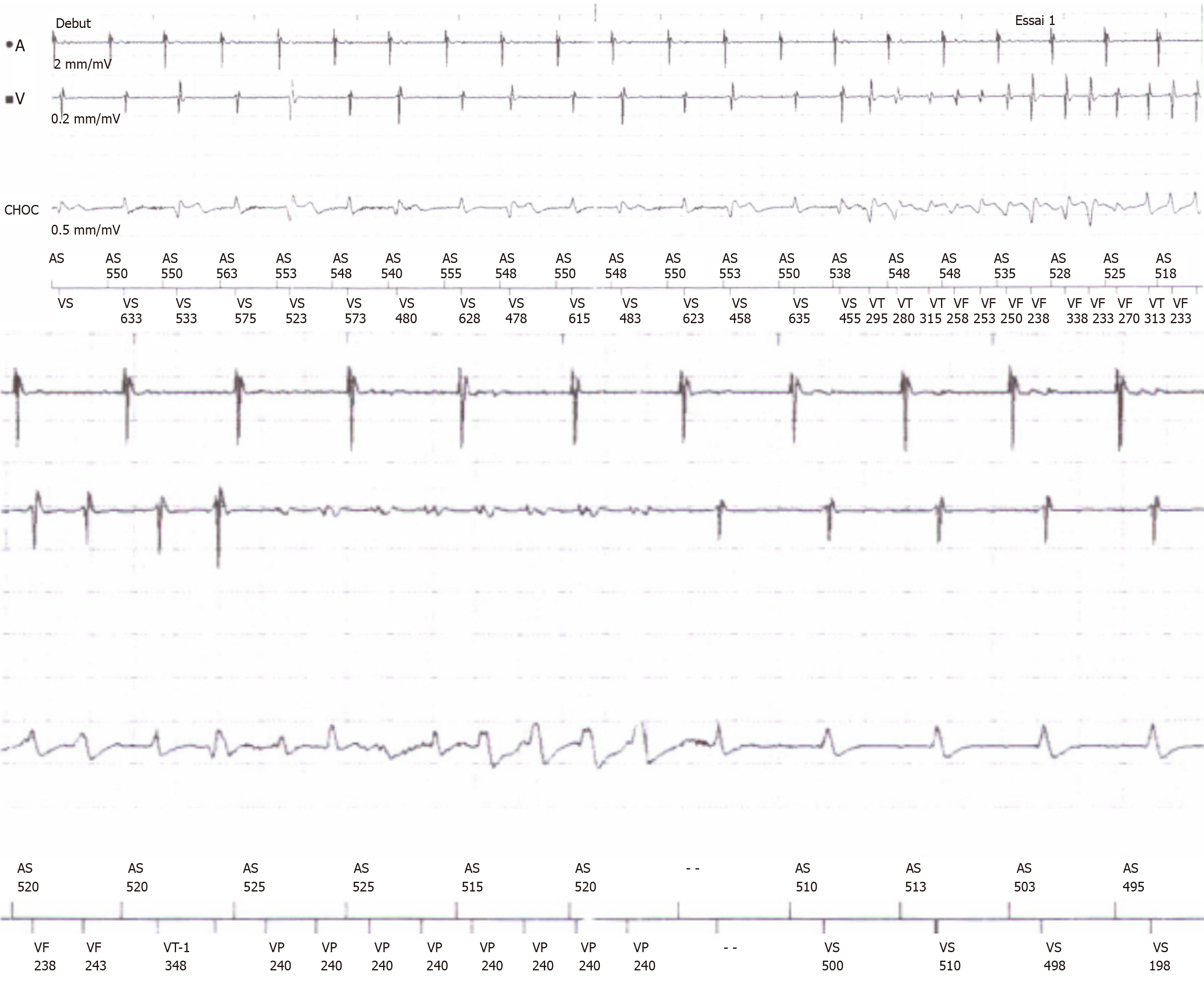
The key is comparison to the last EKG and echocardiogram obtained:.Echocardiography may reveal a new wall motion abnormality.Troponin may re-elevate, but this is often difficult to discern in the context of previously elevated troponin values.Type-II MI due to another aggravating factor (e.g., anemia, hemorrhage).In-stent thrombosis may cause severe transmural infarction.Recurrent ischemic symptoms (e.g., anginal chest pain).If the effusion is >1 cm large or enlarging, consider discontinuation of anticoagulation (to reduce the risk of hemorrhagic pericarditis).Colchicine is often recommended in the absence of any contraindications (e.g., liver disease, renal insufficiency).A proton pump inhibitor should be given to prevent gastric ulceration. First line therapy is high-dose aspirin (e.g., 750-1000 mg Q6-8 hours).Ventricular free wall rupture (may be suggested by pericardial effusion >1 cm).Lab evaluation may show leukocytosis (which is neither sensitive nor specific).CXR may reveal pleural effusion and pneumonitis.Echocardiogram may reveal pericardial effusions (although these may also occur in the absence of pericarditis).Auscultation may reveal pericardial friction rub.Radiation to trapezius ridge supports pericarditis.Chest pain, typically pleuritic ( different in quality from original ischemic pain).Occurs between one week to three months after MI.This may solely include pericarditis, or it may involve a combination of pericarditis plus pleural effusions (pleuropericarditis). Theoretically this is a third-line treatment, if all else fails.Īlso known as Dressler's Syndrome, or post-cardiac injury syndrome (although these terms include other causes such as post-CABG pericarditis).Rather, with conservative management most bleeds will tamponade eventually. Most patients don't require interventional therapy.Perhaps the most important indication for intervention is ongoing extravasation of blood seen on CT scan.Techniques will vary depending on the nature of the bleed, but may include coil embolization or placement of a covered stent. 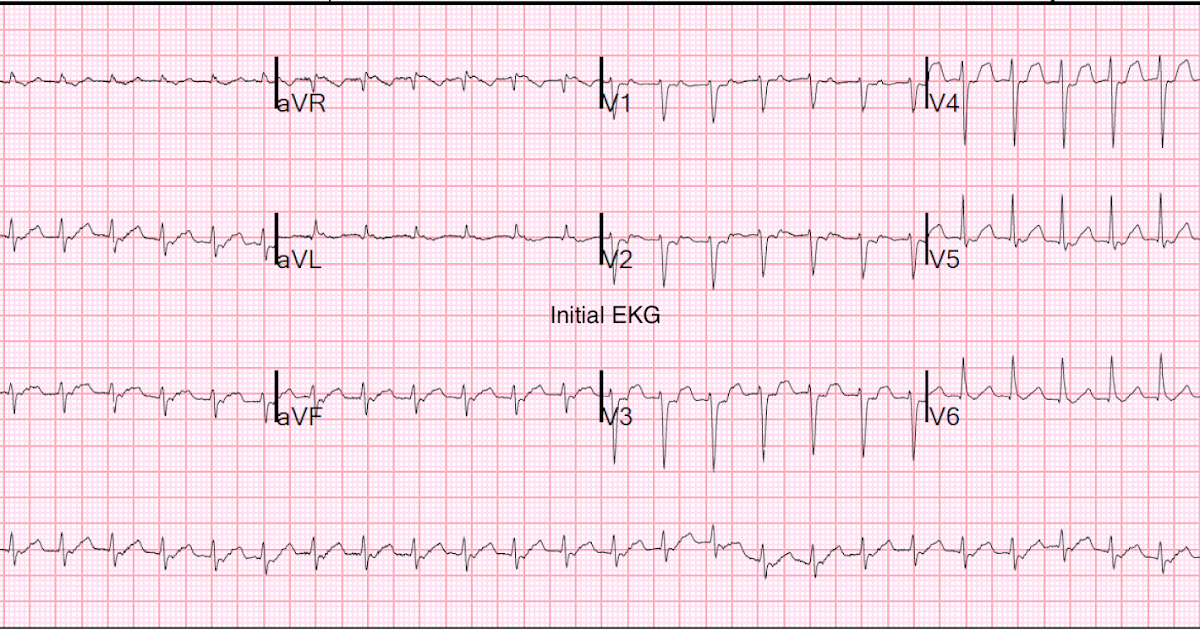
Definitive control can generally be achieved by interventional radiology or interventional cardiology.For hemorrhagic shock, anticoagulation reversal may be considered (although this must be weighed against the risk of coronary stent thrombosis). Interruption of anticoagulation (e.g., if patient on a heparin infusion).PRBC transfusion (type & cross-match, stay 2-4 units ahead).(1) Supportive measures should be instituted without delay:.Merely identifying the hemorrhage isn't helpful, as this doesn't guide the next step in management. Performing a non-angiogram CT scan has little or no value.CT angiogram – the study should be specifically protocoled to evaluate for active extravasation.Bleeding elsewhere (e.g., gastrointestinal bleed due to anticoagulation).Can present as jaundice and abnormal liver function tests (elevated lactate dehydrogenase, AST, and unconjugated bilirubin).Less severe hematoma may present in a delayed fashion, with falling hemoglobin and hematoma tracking over abdomen/flank.Pain may occur in the abdomen, back, or flank.Severe hemorrhage manifests with hypotension and/or shock. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |


 RSS Feed
RSS Feed
